
« Neuro-Oncology is above all a multidisciplinary approach at the centre of which the quality of life of the patient is crucial »
How we treat brain tumours
The Institut Jules Bordet treats both primary brain cancers and brain metastases. Medical imaging plays a major role in this treatment because, in the brain, accurate definition of the tumour is crucial.
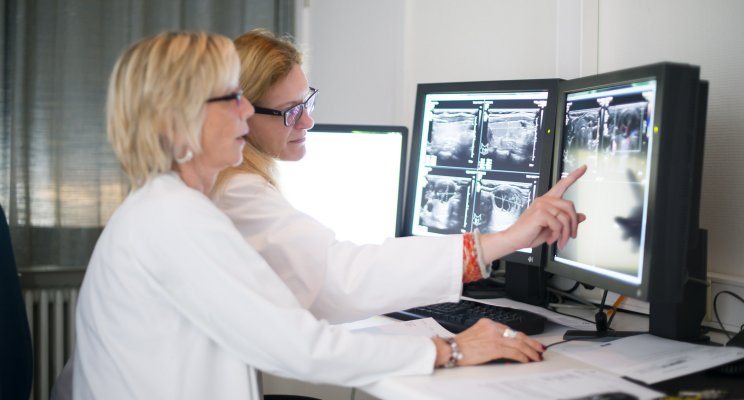
- A CT scan is often the first examination carried out when a brain tumour is suspected.
- Magnetic resonance imaging (MRI) is the reference examination. An MRI detects small lesions and produces different types of images, making it possible to visualise the tumour perfectly.
- A PET scan (positron emission tomography) is used during the diagnostic phase to detect any metastases of a cancer originating in another organ and to guide a biopsy during the therapeutic phase, to determine the precise extent of a surgical resection and in radiotherapy sessions. The Institut Jules Bordet has been a pioneer in the use of PET scan guidance. In some cases, the patient is given an amino acid PET scan (methionine) at the Hôpital Erasme. With this examination it is possible to visualise a heterogeneous tumour and to identify the most aggressive zones.
Depending on the case, treatments are offered either individually, in combination or in succession.
- Surgery is often the first treatment offered, either in order to refine the diagnosis using anatomo-pathological sample analysis (biopsy), or in order to remove the tumour.
- Using GammaKnife© radiosurgery, a single dose of radiotherapy can be delivered in a single session directly to the tumour and without opening the cranium.
- Sessions of radiotherapy and/or adjuvant chemotherapy may be administered after surgery.
Surgical treatments and GammaKnife© radiosurgery are carried out at the Hôpital Erasme in close collaboration between the neurosurgical (Hôpital Erasme) and radiotherapy (Institut Jules Bordet) teams at the two facilities.

The Neurooncological Multidisciplinary Oncology Team at the Institut Jules Bordet is made up of neurosurgeons, oncologists, radiotherapists, nuclear medicine specialists, radiologists, a cancer care coordinator nurse and a cancer psychologist. The team meets every week to decide the best therapeutic strategy to offer each patient while limiting the toxicity (secondary effects) of certain treatments to the maximum. The patient is always informed of these risks. Sometimes alternatives are possible.

The Institut Jules Bordet's nurses, most of whom specialise in oncology, are committed to caring for patients with thought, humanity and professionalism.
Their role does not stop at care and treatment follow-up; they also meet families, and try to be as available as possible and by patients' sides while being attentive to everything confided in them. The role of education, information and support is an integral part of their profession.
They must have relational, technical and scientific skills in line with the gravity and the complexity of the cancerous pathology. The nurses are particularly attentive to the treatment of pain and other symptoms resulting from cancer treatment.
They also focus on their role as trainers to welcome and supervise students, and give them incentive to practice the profession in the best possible conditions.
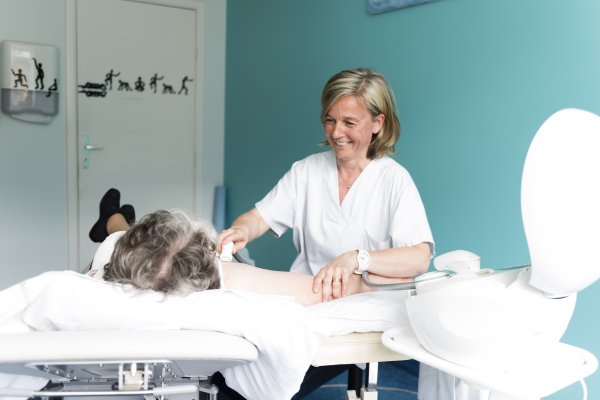
With the medical teams, many other healthcare professionals support the patients. They are dedicated to help patients in managing their illness and treatments, and to promote their wellbeing.
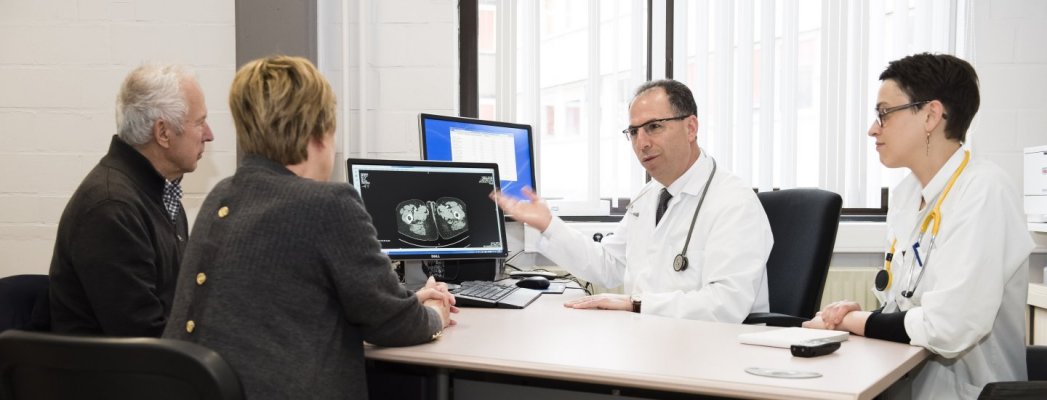
Every year many patients want to request a second medical opinion from our multidisciplinary teams.
Not all the doctors and hospitals will necessarily have the expertise, experience and/or equipment needed for an optimal approach to all types of cancer. At the Jules Bordet Institute this is our job! Requesting a second medical opinion is therefore often useful and reassuring for the patient. This is especially true in the case of rare cancers and/or cancers requiring complex or innovative treatment.
- To request a second opinion for a brain tumour: Tel: +32 (0)2 541 37 23
- To find out more about a second opinion, see our page "second opinion"

The aims of post-cancer care are multiple:
- to keep an eye on the physical and psychological state of the patient
- to manage any medium or long-term secondary effects of certain treatments
- to detect any recurrence as soon as possible
- to identify any new cancer.
Recurrence means that cancer cells reappear after a period of remission that can vary from a few months to several years. It can also happen that the same patient develops different cancers several years apart. In all these cases, the earlier a recurrence or cancerous disease is detected, the faster a new therapeutic strategy can be offered.