How we treat rare tumours
Rare tumours account for around a quarter of the cancers treated at the Institut Jules Bordet. These cancers require very particular and multidisciplinary treatment.
A tumour is described as rare when it affects fewer than 6 people in 100,000. It may appear in an organ or in tissue that is only very rarely affected by cancer (eg: the salivary glands, the penis, etc), or may be situated in an organ where cancer is relatively common but show cell characteristics that are different from those usually observed.
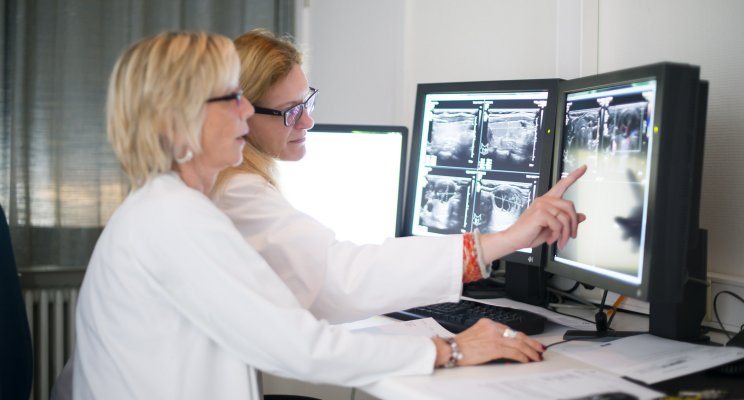
The examinations required to confirm and refine a rare tumour diagnosis are numerous and depend on its location and its type.
Ultrasound, CT scan, MRI, PET scan (positron emission tomography) and endoscopy may be required. But it is the anatomo-pathological tumour sample analysis (biopsy via surgery) that gives the rare tumour diagnosis by revealing a very unusual type of cancer cells. This means that the expertise of pathologists is crucial in this type of diagnosis and it is not unusual for anatomo-pathologists at the Institut Jules Bordet to work together with other major anatomo-pathology laboratories in Belgium and abroad to provide expertise in determining the diagnosis and sending samples for second opinions.
Analysis of the tumour genome using molecular biology and DNA sequencing techniques carried out by pathologists can help guide oncologists in deciding upon a particular treatment.
“As rare and exceptional tumours each affect only a small number of patients, they are little dealt with in medical literature”, explains oncologist Dr Ahmad Awada. “Consequently, their treatment is not always well determined in the guidelines”. In other words, unlike common cancers, there is no consensus on the treatments to be put in place for certain rare tumours. “But just because a cancer is rare, it doesn’t mean that the patient’s prognosis is necessarily poor!” Dr Awada continues. “It all depends on the type and stage of the cancer, the patient’s state of health, the expertise of the medical team, etc. Some rare tumours respond very well to the treatments offered.”

Thanks to the expertise of its medical teams, all the multidisciplinary oncology groups at the Institut Jules Bordet treat rare cancers. However, a special care path has been put in place for very rare cancers (a few cases per year). The Exceptional Tumour Team includes medical oncologists, pathologists, surgeons, radiotherapists and other specialist doctors. “Our first objective is to offer the patient a therapeutic strategy”, Dr Awada explains. “If the tumour is so rare that there is no therapeutic protocol in place for it or if it has not reacted positively to the original treatments the doctors have offered, we need to think afresh. This means doing further in-depth analyses, trying new treatments and experimental approaches, inviting patients to take part in a clinical study that may potentially be beneficial to them, etc”.
The Institut Jules Bordet has a number of doctors whose expertise is internationally recognised. “But we don’t hesitate to call upon external national or international experts to get their opinion on complex cases”, Dr Awada explains. “We are also part of several expert networks, include the European EURACAN network which aims to share expertise and to study rare cancers.”
The Exceptional Tumours Multidisciplinary Oncology Team lists all the rare tumours treated at the Institut Jules Bordet and follows the evolution of patients over time. This paves the way for advanced research and statistical, epidemiological and even clinical studies of new treatments. The ultimate aim being to extract recommendations and guidelines from this which are often lacking in cases of rare and exceptional cancers.

The Institut Jules Bordet's nurses, most of whom specialise in oncology, are committed to caring for patients with thought, humanity and professionalism.
Their role does not stop at care and treatment follow-up; they also meet families, and try to be as available as possible and by patients' sides while being attentive to everything confided in them.
The role of education, information and support is an integral part of their profession.
They must have relational, technical and scientific skills in line with the gravity and the complexity of the cancerous pathology.
The nurses are particularly attentive to the treatment of pain and other symptoms resulting from cancer treatment.
They also focus on their role as trainers to welcome and supervise students, and give them incentive to practice the profession in the best possible conditions.
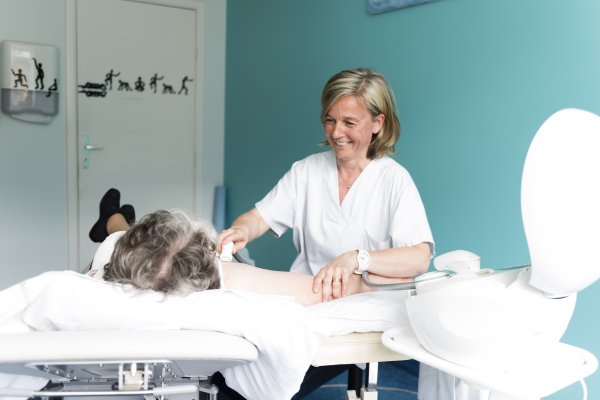
With the medical teams, many other healthcare professionals support the patients. They are dedicated to help patients in managing their illness and treatments, and to promote their wellbeing.
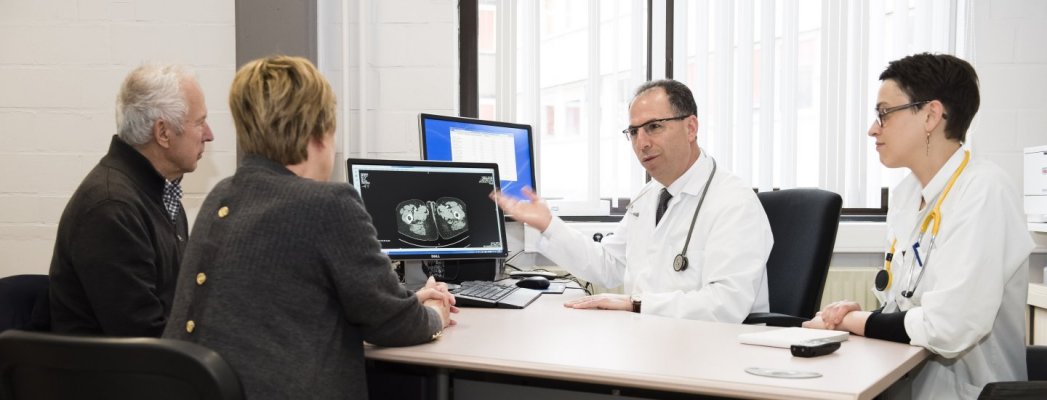
Every year many patients want to request a second medical opinion from our multidisciplinary teams.
Not all the doctors and hospitals will necessarily have the expertise, experience and/or equipment needed for an optimal approach to all types of cancer. At the Jules Bordet Institute this is our job! Requesting a second medical opinion is therefore often useful and reassuring for the patient. This is especially true in the case of rare cancers and/or cancers requiring complex or innovative treatment.
- To request a second opinion for a rare tumour:
Tel: +32 (0)2 541 73 99 - To find out more about a second opinion, see our page "second opinion"

The aims of post-cancer care are multiple:
- to keep an eye on the physical and psychological state of the patient
- to manage any medium or long-term secondary effects of certain treatments
- to detect any recurrence as soon as possible
- to identify any new cancer.
Recurrence means that cancer cells reappear after a period of remission that can vary from a few months to several years. It can also happen that the same patient develops different cancers several years apart. In all these cases, the earlier a recurrence or cancerous disease is detected, the faster a new therapeutic strategy can be offered.