“The therapeutic strategy depends on the type of cancer, its extent and the patient’s general state of health.”
How we treat cancers of the lungs and thoracic cavity
Thanks to extensive internal and external collaboration, the Institut Bordet is able to treat all cancers of the thoracic cavity, including lung cancer.
Several types of cancer can develop in the thorax: small and large cell lung (or “bronchial”) cancer, pulmonary metastases originating in other primary tumours and rare tumours such as cancer of the thymus, mesothelioma, pleura, etc.
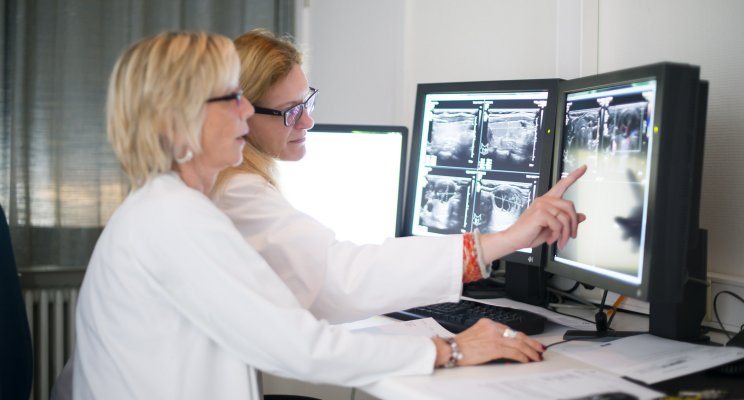
The diagnostic phase is divided into 3 parts, generally carried out concurrently:
- A biopsy to reveal the nature of the tumour. In the case of bronchial tumours, this tissue sample is usually removed via a bronchoscopy for bronchial tumours.
- Medical imaging examinations aimed at establishing the extent (stage) of the cancer and to look for any possible metastases. The patient may have a thoracic CT (computerised tomography) scan, a PET scan (positron emission tomography), MRI scan, etc.
- Cardiac, respiratory (pulmonary function) and blood function tests to help determine the patient’s fitness to undergo the different types of treatment.
The therapeutic strategy is discussed by the Institut Bordet Thoracic Multidisciplinary Cancer Care Team (CMO). The team includes oncologists, surgeons, radiotherapists, nuclear medicine specialists, pathologists, a cancer psychologist and cancer care coordinator nurse.
The principal treatments are:
- Drugs (chemotherapy, targeted therapies and immunotherapy). Conventional chemotherapy may be administered as part of combined treatment including surgery and/or radiotherapy. Doctors at the Institut Bordet Thoracic Cancer Clinic belong to a number of international networks, enabling them to access innovative treatments as part of clinical studies.
- Surgery: surgery is carried out at the thoracic surgery department of the Erasmus hospital.
- Radiotherapy: a number of techniques (for example, stereotaxic radiotherapy) are available at the Institut Bordet in order to target the tumour more effectively and avoid secondary effects.

The Institut Jules Bordet's nurses, most of whom specialise in oncology, are committed to caring for patients with thought, humanity and professionalism.
Their role does not stop at care and treatment follow-up; they also meet families, and try to be as available as possible and by patients' sides while being attentive to everything confided in them.
The role of education, information and support is an integral part of their profession.
They must have relational, technical and scientific skills in line with the gravity and the complexity of the cancerous pathology.
The nurses are particularly attentive to the treatment of pain and other symptoms resulting from cancer treatment.
They also focus on their role as trainers to welcome and supervise students, and give them incentive to practice the profession in the best possible conditions.
Patients who smoke and would like help to quit smoking are given support to do this. A specialist “occupational disease” consultation is available for patients affected by thoracic cancer. Some cancers can be caused by toxins (asbestos, heavy metals, etc) present in certain occupational sectors. If exposure is confirmed, these patients can make a claim to the Fonds des Maladies Professionnelles (www.fmp-fbz.fgov.be).
As well as our medical teams, the Institut Bordet has many other healthcare professionals to support our out-patients and in-patients. They are there to help patients manage their illness, treatments and the consequences of treatment in the best possible way.
Every year many patients request a second medical opinion from our multidisciplinary teams.
Here are the essential documents that you must submit to the secretariat BEFORE obtaining an appointment for a second opinion:
- Full and detailed anatomopathological diagnosis (with immunochemical and molecular analyses if obtained)
- Results of additional examinations carried out with images (CD-ROM or Internet link with access code).
- Scanner/NMRRMN
- Pet Scan
- Bronchoscopy
- Lung function tests
- Cardiac examinations (ECG, echography, opinion, etc.)
- Biology
- Other
- If you have already received treatment:
- Dates of start and end of treatment
- Details of treatment (chemotherapy, radiotherapy, etc.)
- If surgery, detailed protocol
- Insofar as possible, a summary of the oncological past (consultation note, Multidisciplinary Oncology Team, summary of hospitalisations, etc.). The full copy of the medical file is not required.
- If the request for a second opinion comes from abroad, the documents in the medical file must be translated into French, Dutch or English

The aims of post-cancer care are multiple:
- to keep an eye on the physical and psychological state of the patient
- to manage any medium or long-term secondary effects of certain treatments
- to detect any recurrence as soon as possible
- to identify any new cancer.
Recurrence means that cancer cells reappear after a period of remission that can vary from a few months to several years. It can also happen that the same patient develops different cancers several years apart. In all these cases, the earlier a recurrence or cancerous disease is detected, the faster a new therapeutic strategy can be offered.