How we treat bone and soft tissue cancers
The medical team at the Institut Jules Bordet treats tumours that appear in the soft tissue (muscles, fat, nerves, blood vessels, etc), primary bone cancer in children (in close collaboration with HUDERF – the Hôpital Universitaire des Enfants Reine Fabiola) and in adults as well as bone metastases.
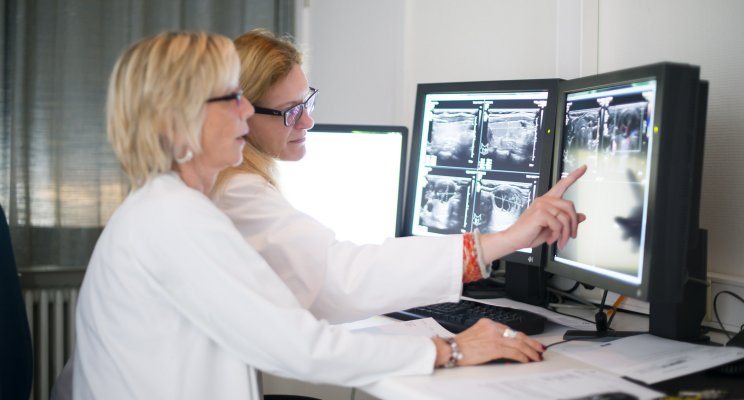
After an initial assessment using radiography or ultrasound, diagnosis needs to be further refined using 3 types of examination:
- The patient may undergo an MRI, a CT scan and/or a bone scintigraphy.
- A biopsy of the bone or soft tissue tumour is taken by direct puncture using an ultrasound or scan-guided tru-cut device to remove a small tumour sample, or via a larger surgical removal.
- A scan assessment of the lungs and abdomen to establish the extent of the cancer and a PET scan to look for any possible metastases.
Neoadjuvant chemotherapy is carried out prior to resection of the primary tumour. The aim is reduce the size of the tumour and make it easier to operate on. Chemotherapy also attacks micrometastases that can sometimes already be present in other organs. The Jules Bordet Institute was a pioneer in the development of chemotherapy protocols for bone tumours in children and soft tissue tumours in adults.
The purpose of surgery is to resect the whole tumour while avoiding amputation as far as possible.
Adjuvant radiotherapy is indicated in certain soft tissue cancers and is often carried out in the palliative treatment of bone metastases.
The Institut Jules Bordet Orthopaedic Oncology Surgery Department offers different types of bone loss reconstruction, secondary to surgery, in children, in close collaboration with HUDERF.
- In adults, skeletal reconstruction is principally by means of prosthesis.
- In children, a growth prosthesis is generally preferred, enabling the size of the prosthesis to develop with the child’s rate of growth.
- If the area of operation is in the middle of a functional bone (humerus, femur, tibia, etc), bone reconstruction can be by means of an autograft (transplant from the patient’s fibula) or an allograft.
- In exceptional cases, skeletal reconstruction may reuse resected bone as an allograft, after eliminating all cancerous tissue by a procedure similar to pasteurisation.
The Institut Jules Bordet also treats the after-effects of certain cancer treatments in the bone system.

The Soft Tissue and Bone Multidisciplinary Oncology Team includes surgeons, orthopaedists, medical oncologists, pathologists, radiologists, nuclear medicine specialists, radiotherapists, physiotherapists, cancer psychologists and a cancer care coordinator nurse. The team meets every week to discuss the medical situation of each patient and determine the most appropriate therapeutic strategy.

The Institut Jules Bordet's nurses, most of whom specialise in oncology, are committed to caring for patients with thought, humanity and professionalism.
Their role does not stop at care and treatment follow-up; they also meet families, and try to be as available as possible and by patients' sides while being attentive to everything confided in them. The role of education, information and support is an integral part of their profession.
They must have relational, technical and scientific skills in line with the gravity and the complexity of the cancerous pathology. The nurses are particularly attentive to the treatment of pain and other symptoms resulting from cancer treatment.
They also focus on their role as trainers to welcome and supervise students, and give them incentive to practice the profession in the best possible conditions.
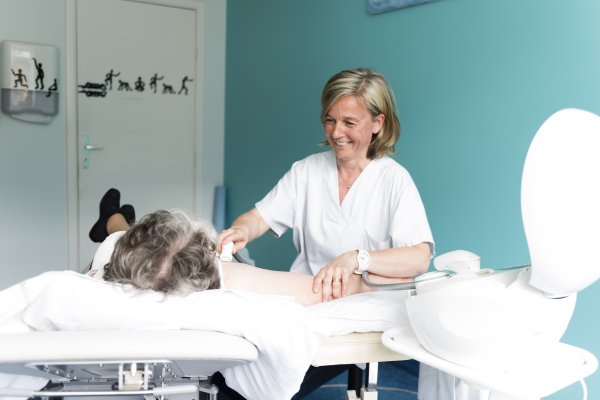
With the medical teams, many other healthcare professionals support the patients. They are dedicated to help patients in managing their illness and treatments, and to promote their wellbeing.
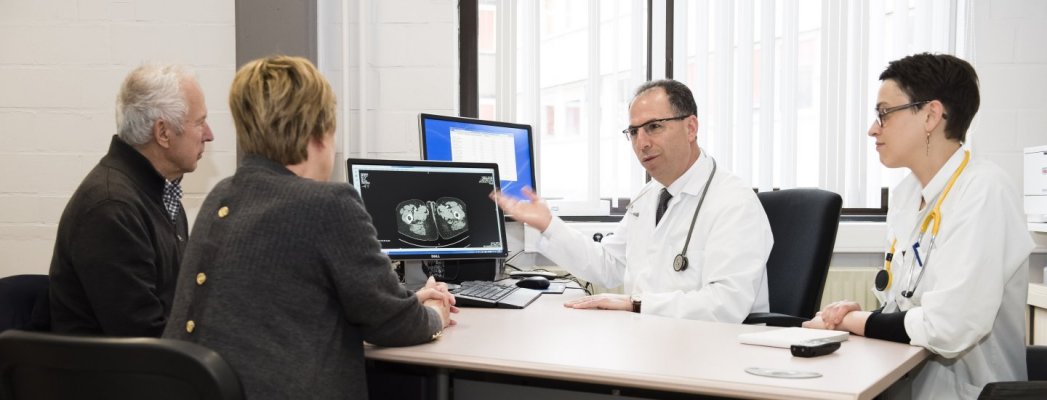
Every year many patients want to request a second medical opinion from our multidisciplinary teams.
Not all the doctors and hospitals will necessarily have the expertise, experience and/or equipment needed for an optimal approach to all types of cancer. At the Jules Bordet Institute this is our job! Requesting a second medical opinion is therefore often useful and reassuring for the patient. This is especially true in the case of rare cancers and/or cancers requiring complex or innovative treatment.
- To request a second opinion for a cancer of bone and soft tissue: Tel: +32 (0)2 541 39 99
- To find out more about a second opinion, see our page "second opinion"

The aims of post-cancer care are multiple:
- to keep an eye on the physical and psychological state of the patient
- to manage any medium or long-term secondary effects of certain treatments
- to detect any recurrence as soon as possible
- to identify any new cancer.
Recurrence means that cancer cells reappear after a period of remission that can vary from a few months to several years. It can also happen that the same patient develops different cancers several years apart. In all these cases, the earlier a recurrence or cancerous disease is detected, the faster a new therapeutic strategy can be offered.