
“A surgeon never takes the decision to operate on their own. The management of hepatic tumours is always multidisciplinary.”
How we treat liver cancers
There are 2 types of hepatic cancer: primary liver cancer and hepatic metastases originating from other primary tumours. Surgery is the major treatment for these cancers but it is limited by the need to conserve sufficient functional liver tissue. Other therapies may be combined with surgery.
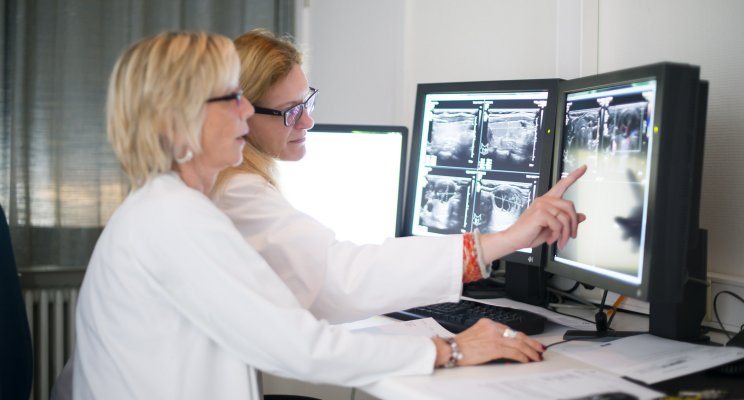
Medical imaging examinations (CT scan, MRI and PET scan) aim to locate hepatic tumours accurately and establish the surgical strategy to follow. The “resectability” of the tumour has to be confirmed. Can the tumour be completely removed while conserving sufficient functional liver tissue? This is the challenge in achieving a curative treatment!
The patient also undergoes other examinations and tests (blood analysis, cardiac and respiratory assessment, etc) to evaluate his general state of health.

Hepatic tumour resection is at the centre of the therapeutic strategy for liver cancer. It is often combined with other treatments, before or after surgery.
The Institut Bordet Liver Tumour Multidisciplinary Cancer Care Team (CMO) meets every week and includes surgeons, gastroenterologists, medical oncologists, radiologists, nuclear medicine specialists, pathologists, a cancer psychologist and a cancer care nurse coordinator (ICSO). The purpose is to discuss each patient’s situation in a collaborative way.
Various treatments may be combined with surgery:
- chemotherapy
- external radiotherapy
- intra-arterial radiotherapy (radioembolisation). This treatment involves injecting radioactive microspheres into the tumour to irradiate it from within. The Institut Bordet was a pioneer in developing radioembolisation treatments
- radiofrequency uses radio waves introduced into the tumour to “burn” the cancer cells through high frequency ultrasound.
At the Institut Bordet, a combination of several treatments and surgical techniques is always considered. These complex, multidisciplinary approaches aim to improve results and the rate of cure. They enable radical surgical procedures to be carried out in patients with advanced stage hepatic cancer and can make it possible to operate on patients who were originally inoperable because of the number of hepatic lesions, their size or their location.
In some cases, curative surgery is made possible by combining several pre-operative treatments and/or techniques such as chemotherapy, radioembolisation and portal vein embolization techniques which induce atrophy (reduction) of the part of the liver to be resected and hypertrophy of the residual part to compensate for functional deficit, etc.

The Institut Jules Bordet's nurses, most of whom specialise in oncology, are committed to caring for patients with thought, humanity and professionalism.
Their role does not stop at care and treatment follow-up; they also meet families, and try to be as available as possible and by patients' sides while being attentive to everything confided in them. The role of education, information and support is an integral part of their profession.
They must have relational, technical and scientific skills in line with the gravity and the complexity of the cancerous pathology. The nurses are particularly attentive to the treatment of pain and other symptoms resulting from cancer treatment.
They also focus on their role as trainers to welcome and supervise students, and give them incentive to practice the profession in the best possible conditions.
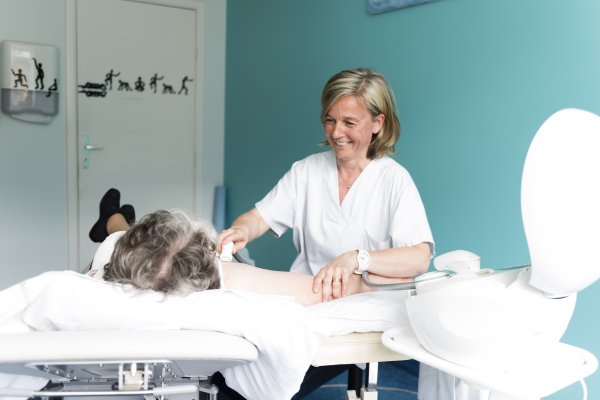
With the medical teams, many other healthcare professionals support the patients. They are dedicated to help patients in managing their illness and treatments, and to promote their wellbeing.
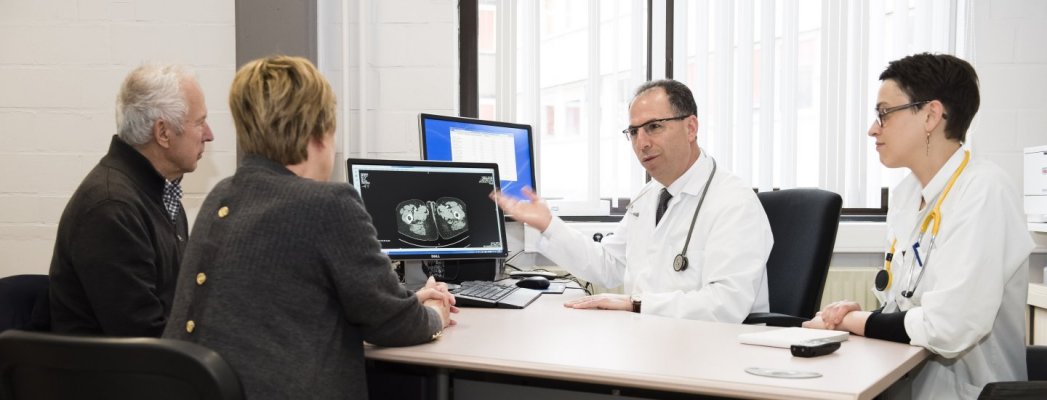
Every year many patients want to request a second medical opinion from our multidisciplinary teams.
Not all the doctors and hospitals will necessarily have the expertise, experience and/or equipment needed for an optimal approach to all types of cancer. At the Jules Bordet Institute this is our job! Requesting a second medical opinion is therefore often useful and reassuring for the patient. This is especially true in the case of rare cancers and/or cancers requiring complex or innovative treatment.
- To request a second opinion for a hepatic cancer: Tel: +32 (0)2 541 34 80
- To find out more about a second opinion, see our page "second opinion"

The aims of post-cancer care are multiple:
- to keep an eye on the physical and psychological state of the patient
- to manage any medium or long-term secondary effects of certain treatments
- to detect any recurrence as soon as possible
- to identify any new cancer.
Recurrence means that cancer cells reappear after a period of remission that can vary from a few months to several years. It can also happen that the same patient develops different cancers several years apart. In all these cases, the earlier a recurrence or cancerous disease is detected, the faster a new therapeutic strategy can be offered.