How we treat gynaecological cancers
The term gynaecological cancer covers cancers of the endometrium, the ovaries, the cervix, the vulva and the vagina. These intimate cancers require multidisciplinary, personalised care and treatment.
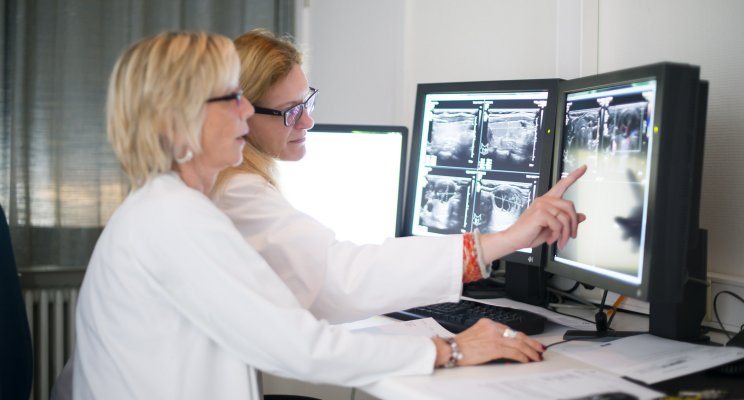
The examinations needed to establish an accurate diagnosis of gynaecological cancer depend on the organ or tissue concerned. In all cases, the following are standard:
- magnetic resonance imaging (MRI) of the pelvis;
- a biopsy of the suspicious tissue;
- in ovarian cancer, if the patient has a personal or family history of breast cancer, a genetic mutation may be looked for.
Depending on the individual case, these examinations may be supplemented by an endoscopy (of the colon, the bladder, etc), a CT scan, and an abdominal ultrasound to establish the extent of the tumour and detect any possible metastases.

The Gynaeco-Mammary Breast Clinic at the Institut Jules Bordet also treats gynaecological cancers. Medical oncologists, gynaecologists, surgeons, radiotherapists, pathologists, a cancer psychologist and a cancer care coordinator nurse meet regularly to discuss each patient’s situation and offer individualised treatment.
As with breast cancer, patients affected by a gynaecological cancer are offered specialised support: intimacy consultation, psychological support, creative workshops, etc.
The therapeutic strategy for managing gynaecological cancer depends on the type and site of the cancer, its possible spread and the patient’s general state of health.
Surgery is necessary in most cases of gynaecological cancer. This involves the removal of all or part of the organ or tissue where the tumour is located. The surrounding lymph nodes may also be removed, along with certain neighbouring organs such as the uterus, ovaries, etc.
The Institut Jules Bordet has played a key role in the development of the sentinel lymph node technique, used in breast cancer, vulval cancer and other cancers.
The Institut Jules Bordet has also been a pioneer in minimally invasive surgery using endoscopy and Da Vinci® robot-assisted surgery. These surgical techniques are the preferred option in endometrial and cervical cancer.
Depending on the case, surgery for gynaecological cancer may be preceded or supplemented by chemotherapy and/or radiotherapy.
In ovarian cancer, “intraperitoneal” (inside the peritoneal cavity) chemotherapy may be administered during surgery.

The Institut Jules Bordet's nurses, most of whom specialise in oncology, are committed to caring for patients with thought, humanity and professionalism.
Their role does not stop at care and treatment follow-up; they also meet families, and try to be as available as possible and by patients' sides while being attentive to everything confided in them. The role of education, information and support is an integral part of their profession.
They must have relational, technical and scientific skills in line with the gravity and the complexity of the cancerous pathology. The nurses are particularly attentive to the treatment of pain and other symptoms resulting from cancer treatment.
They also focus on their role as trainers to welcome and supervise students, and give them incentive to practice the profession in the best possible conditions.
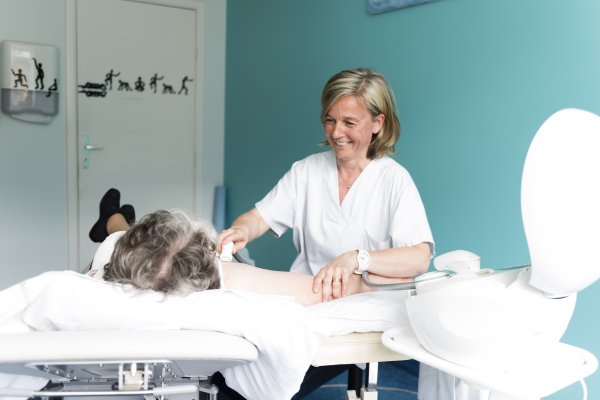
With the medical teams, many other healthcare professionals support the patients. They are dedicated to help patients in managing their illness and treatments, and to promote their wellbeing.
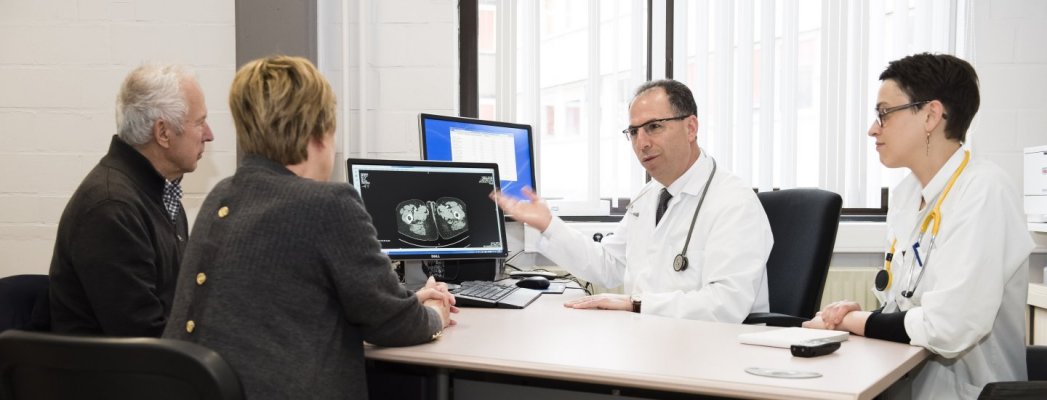
Every year many patients want to request a second medical opinion from our multidisciplinary teams.
Not all the doctors and hospitals will necessarily have the expertise, experience and/or equipment needed for an optimal approach to all types of cancer. At the Jules Bordet Institute this is our job! Requesting a second medical opinion is therefore often useful and reassuring for the patient. This is especially true in the case of rare cancers and/or cancers requiring complex or innovative treatment.
- To request a second opinion for a gynecological cancer:
- BEFORE surgery : Tel: +32 (0)2 541 34 58
- AFTER surgery : Tel: +32 (0)2 541 73 99
- To find out more about a second opinion, see our page "second opinion"

The aims of post-cancer care are multiple:
- to keep an eye on the physical and psychological state of the patient
- to manage any medium or long-term secondary effects of certain treatments
- to detect any recurrence as soon as possible
- to identify any new cancer.
Recurrence means that cancer cells reappear after a period of remission that can vary from a few months to several years. It can also happen that the same patient develops different cancers several years apart. In all these cases, the earlier a recurrence or cancerous disease is detected, the faster a new therapeutic strategy can be offered.
ESGO accreditation

The Institut Jules Bordet is the second Belgian centre to obtain ESGO accreditation for the treatment of locally advanced ovarian cancer. This is a recognition of the quality and excellence of the treatment of this type of cancer at the Institute. The accreditation, obtained in July 2025, is based on very strict criteria assessing, in particular, the surgical management of a minimum number of cases of locally advanced ovarian cancer per year, the presentation of files to the gynaecological Multidisciplinary Oncology Consultations (CMO). In addition, the team must include surgeons with expertise in performing macroscopically complete cytoreduction surgery (debulking).
Scientific studies have shown that centres that meet these quality criteria for the management of patients with locally advanced ovarian cancer have a better chance of patient survival. ESGO, the European Society of Gynaecological Oncology, is an organisation of over 3,400 professionals worldwide, dedicated to ensuring excellence in the care of women with gynaecological cancers.
Patients treated at an ESGO-accredited centre have a better chance of recovery.