How we treat thyroid cancers
The Institut Jules Bordet treats all types of thyroid cancer. The great majority can be cured but require correct assessment of the risk of recurrence and follow-up care for life.
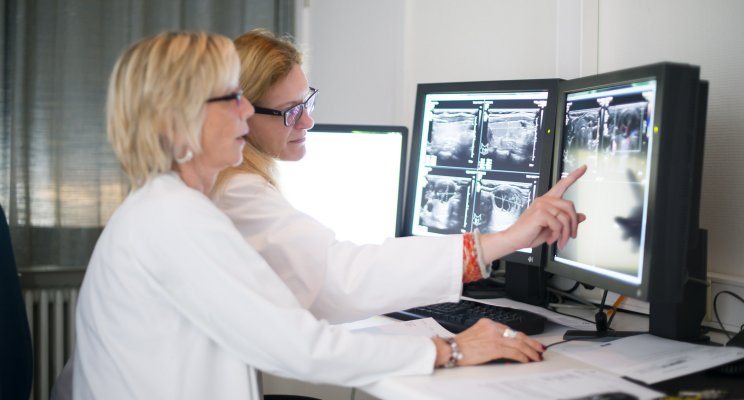
To determine if a thyroid nodule (“lump”) is cancerous, first an ultrasound is done to assess the size and structure of the nodule(s) and a blood sample is taken to measure the thyroid hormones.
A thyroid scintigraphy may be carried out in some cases. But it is the biopsy, ie the removal of a fragment of the nodule and laboratory analysis of this sample that will determine a cancer diagnosis.
Surgery is the first-line treatment for thyroid cancer. It involves total or partial ablation of the thyroid gland and, possibly, of the neighbouring lymph nodes.
The operation depends on the size of the tumour, the risk factors and the possible extent of the cancer. In all cases, what is removed undergoes laboratory analysis.
According to the level of risk of persistence or recurrence of the cancer, there are 2 possibilities for follow-up care:
- a low risk may mean simply an annual or 6-monthly check-up
- when the risk of persistence or recurrence is higher, a more detailed check-up is needed. In some cases, additional treatment is offered. This is generally a nuclear medicine treatment, using radioactive iodine.
Multiple doses of radioactive iodine, radiotherapy, further surgery or other local treatments may be indicated in the event of recurrence. Chemotherapy is reserved for certain rare and more aggressive thyroid cancers (5% to 15% of cases). The Institut Jules Bordet is part of EURACAN, a European network that studies rare cancers.

The Thyroid Multidisciplinary Oncology Team includes endocrinologists, medical oncologists, cervicofacial surgeons (specialising in the head and neck), pathologists, nuclear medicine specialists, a cancer psychologist and a cancer care coordinator nurse. The team meets to assess each patient’s situation case by case, in order to offer the most appropriate therapeutic strategy.
Patients who have had thyroid cancer must receive lifelong monitoring. This is to detect and treat any possible recurrence and also to manage their hormone replacement therapy. Ablation of the thyroid means that the thyroid hormone thyroxine must be taken for life. This treatment must be adapted to the type and stage of the cancer, but also to other requirements (for example, pregnancy, elderly patient, etc).

The Institut Jules Bordet's nurses, most of whom specialise in oncology, are committed to caring for patients with thought, humanity and professionalism.
Their role does not stop at care and treatment follow-up; they also meet families, and try to be as available as possible and by patients' sides while being attentive to everything confided in them. The role of education, information and support is an integral part of their profession.
They must have relational, technical and scientific skills in line with the gravity and the complexity of the cancerous pathology. The nurses are particularly attentive to the treatment of pain and other symptoms resulting from cancer treatment.
They also focus on their role as trainers to welcome and supervise students, and give them incentive to practice the profession in the best possible conditions.
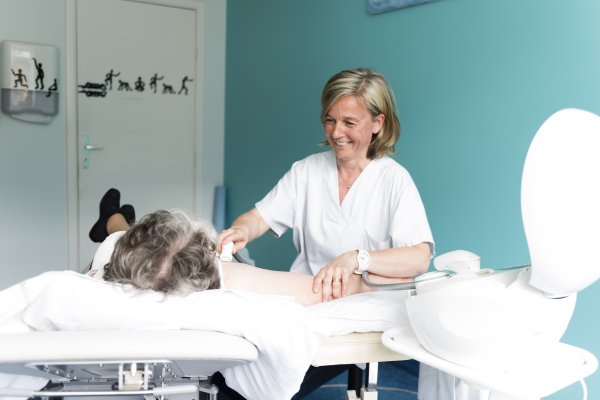
With the medical teams, many other healthcare professionals support the patients. They are dedicated to help patients in managing their illness and treatments, and to promote their wellbeing.
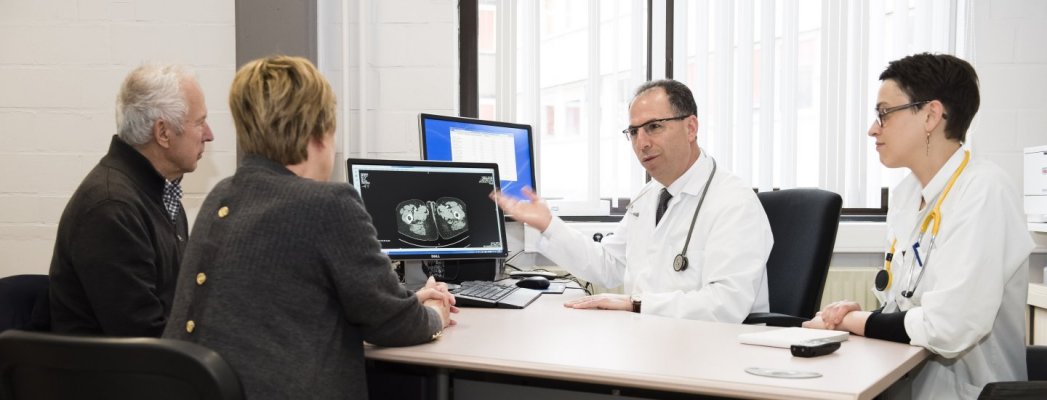
Every year many patients want to request a second medical opinion from our multidisciplinary teams.
Not all the doctors and hospitals will necessarily have the expertise, experience and/or equipment needed for an optimal approach to all types of cancer. At the Jules Bordet Institute this is our job! Requesting a second medical opinion is therefore often useful and reassuring for the patient. This is especially true in the case of rare cancers and/or cancers requiring complex or innovative treatment.
- To request a second opinion for a thyroid cancer: Tel: +32 (0)2 541 34 47
- To find out more about a second opinion, see our page "second opinion"

The aims of post-cancer care are multiple:
- to keep an eye on the physical and psychological state of the patient
- to manage any medium or long-term secondary effects of certain treatments
- to detect any recurrence as soon as possible
- to identify any new cancer.
Recurrence means that cancer cells reappear after a period of remission that can vary from a few months to several years. It can also happen that the same patient develops different cancers several years apart. In all these cases, the earlier a recurrence or cancerous disease is detected, the faster a new therapeutic strategy can be offered.